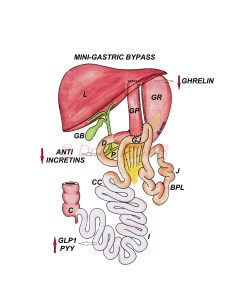
LAPAROSCOPIC BANDED MGB - OAGB
LAPAROSCOPIC BANDED MINI GASTRIC BYPASS - ONE ANASTOMOSIS GASTRIC BYPASS (LAPAROSCOPIC BANDED MGB - OAGB)
– Simplified version of Roux en y gastric bypass for the treatment of severe obesity and severe diabetes.
– More powerful than Gastric sleeve and Roux en y gastric bypass.
– More popular in India because it is simple and more effective.
– Procedure:
- Performed by robotic or laparoscopic method (By putting small holes over the tummy) using advanced high quality imported laparoscopic equipment and instruments.
- Gastric pouch is created using high quality staplers and stapler guns.
- A loose ring is placed around the gastric pouch, with the intention of creating long term restriction.
- Jejunum (Mid small intestine) up to 200 cm beyond the duodenojejunal junction, is attached to this pouch in a loop fashion.
– In India and Asia,
- Individuals suffering from severe obesity with the body mass index is ≥ 32.5 kg/m2 with co-morbid medical conditions such as type 2 diabetes.
- Individuals suffering from severe obesity with the body mass index is ≥ 37.5 kg/m2 even without any co-morbid medical conditions.
– In Western countries
- Individuals suffering from severe obesity with the body mass index is ≥ 35 kg/m2 with co-morbid medical conditions such as type 2 diabetes.
- Individuals suffering from severe obesity with the body mass index is ≥ 40 kg/m2 even without any co-morbid medical conditions.
– Weight loss is mainly due to physiological changes altering body energy balance.
– Because of these changes
- Appetite (Hunger) is reduced.
- Metabolic rate is increased.
- Energy expenditure is increased.
- ‘Fat mass’ is reset to a lower level.
- Fat starts melting as body doesn’t want to store large quantity of fat.
- You don’t eat large quantity of food as you start hating unhealthy foods.
– Diversion of the biliopancreatic juices contribute partly to these physiological changes.
– Role of food restriction and malabsorption is secondary.
– Same physiological changes are responsible for type 2 diabetes remission.
- Insulin resistance is reduced.
- Insulin production is optimised to control blood sugars.
– Since weight loss and diabetes remission are mainly related to physiological changes and role of restriction or malabsorption is secondary, placing a ring around gastric pouch doesn’t offer any extra advantage in terms of weight loss, diabetes remission, prevention of weight regain or diabetes recurrence.
– Average excess weight loss is ~ 70 to 80%.
– Some may lose above average, even 100% of the excess weight loss but that number is less.
– For Example – If you are 50 kg excess weight, you lose approximately 35 to 40 kg on average. Some may lose all the extra 50 kg but that number is less.
– Generally if your weight burden is less, you lose more percentage of excess weight and if your weight burden is more you lose less percentage of excess weight.
– Total weight loss percentage is ~ 30 to 35%.
– Average diabetes remission ~ 70 to 80%.
– It is necessary to follow lifestyle modifications to improve weight loss and diabetes remission and to prevent weight regain and diabetes recurrence.
– Results in long lasting weight loss.
– Results in long lasting diabetes remission.
– Relatively simple and safe surgery.
– When bypassed segment of intestine is less than 200 cm, so malabsorption risk is less.
– Stomach is not removed. So there is ‘at risk gastric remnant’.
– It is not possible to check for ulcer or cancer in remnant stomach by endoscopy.
– It is not possible to access common bile duct (pipe below liver) by endoscopy.
– Duodenum (1st part of intestine) is bypassed, so risk of calcium and iron deficiencies is high.
– Pylorus (valve below stomach controlling food output) is bypassed, so risk of dumping syndrome (dumping of nutrients into intestine leading to fluctuations in blood glucose) is high.
– There is risk of narrowing of anastomosis (attachment between gastric pouch and jejunum).
– There is risk of marginal ulcers (ulcers at the anastomosis).
– Since it is a loop anastomosis (attachment between gastric pouch and jejunum), there is risk of bile reflux into gastric pouch. Long term consequences of this bile reflux are unknown.
– Some may lose below average. Inadequate weight loss ~ 10%. They may lose only 5 to 10 kg and stop losing further.
– Average weight regain ~ 20 to 30%.
– Diabetes recurrence after Banded MGB – OAGB is ~ 30 to 40%.
– Placing a band may at most postpone weight regain or diabetes remission but can’t prevent them.
– Weight regain and diabetes recurrence is less than that of gastric sleeve.
– Banded MGB – OAGB is less powerful, less effective compared to sleeve plus bypass combination procedures such as Sleeve gastrectomy with loop gastroileal bypass (SG LGIB), Single anastomosis duodenoileal bypass with sleeve (SADI S) and BPD DS because bypassed small intestine (biliopancreatic limb) is relatively shorter.
– If anyone regains weight or if diabetes recurs after Banded MGB or OAGB, revision to loop duodenal switch or duodenal switch re-induce significant weight loss and diabetes remission.
– Most of these limitations are addressed by sleeve plus bypass combination surgeries.
– It is very very safe procedure.
– It is a life saving surgery.
– Severe obesity and severe diabetes are dangerous.
– Bariatric and Metabolic surgeries are very safe.
– Complications are very rare. Even if they occur, they can be rectified.
– Band related complications such as band slippage, and band erosion are rare.