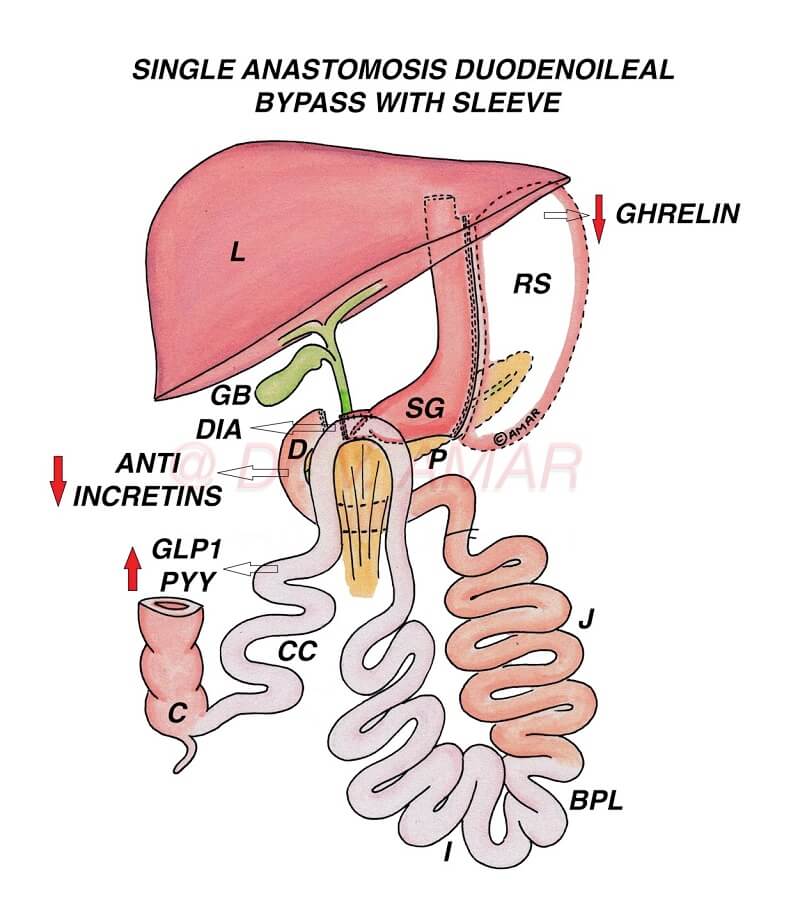
Single Anastomosis Duodenoileal Bypass With Sleeve (SADI S)
Technically it is a loop modification of biliopancreatic diversion with duodenal switch (BPD DS). Gastric sleeve is formed using staplers. First part of small intestine (duodenum) is disconnected and attached to distal ileum (last part of small intestine) in a loop fashion 250 – 350 cm proximal to ileocecal junction (loop duodenoileal anastomosis).
Weight loss after SADI S is mainly because of hormonal and genetic changes. Role of food restriction or mal-absorption is secondary. After this operation Ghrelin hormone levels come down as fundus of the stomach is removed. GLP 1, Peptide YY hormone levels increase as food rapidly enters from 1st part of duodenum into distal ileum. Food doesn’t enter the remaining duodenum, jejunum and proximal ileum. So levels of anti incretin hormones come down. There will be more than 200 hormonal changes after surgery. Removal of body of stomach alters several genes involved in energy balance. These hormonal and genetic changes reduce appetite, increase energy expenditure and reset the ‘fat mass’ to a lower level, resulting in long lasting and effective weight loss. Same hormonal changes are responsible for long lasting type 2 diabetes remission. Ghrelin and anti incretins act against insulin. As levels of these hormones come down, insulin resistance comes down. Since GLP 1 hormone is increased, insulin production increases and insulin resistance comes down. Significant diversion of biliopancreatic juices also contributes to the metabolic effects of this surgery.
Hormonal and genetic changes responsible for long lasting weight loss and durable diabetes remission are very high in SADI S compared to Sleeve gastrectomy (SG), Roux en y gastric bypass (RYGB), Mini gastric bypass – One anastomosis gastric bypass (MGB – OAGB) and Sleeve gastrectomy with loop duodenojejunal bypass (SG LDJB), because bypassed bowel is relatively longer compared to these procedures. So weight loss is more effective & long lasting and diabetes remission is more & durable. Chances of weight regain and diabetes recurrence are very low. SADI S has several advantages compared to RYGB and MGB – OAGB. There is no ‘at risk’ stomach remnant, calcium and iron deficiency risk is low since first 4 cm of duodenum is not bypassed and risk of dumping syndrome is less because of intact pylorus controlling food out put into first part of duodenum, there is no risk of marginal ulcers and risk of internal hernias is low.
Compared to BPD DS, protein-energy malnutrition and malabsorption risk is low because the common channel (intestine available for digestion and absorption) is relatively long.
SADI S is technically complex and time taking compared to SG, RYGB and MGB – OAGB. It needs advanced laparoscopic surgical skills and training. Another disadvantage is loss of endoscopic access to biliary tract (Pathway connecting liver and small intestine). Protein energy malnutrition, malabsorption, foul smelling oily stools, diarrhea and incontinence are high if common channel length is 250 cm or less. These problems are significantly reduced but efficacy remains same when common channel is increased to 300 – 350 cm.